In the last few years, we have seen a flurry of media articles, tweet-a-thons, Facebook posts, and hashtags making the rounds in the run up to World Mental Health Day—calling for attention to an issue that seems to have reached an inflection point. Campaigns such as #SpeakYourMind, #NotAshamed, and #ItsOkToTalk address mental health stigma by broadcasting personal anecdotes from those with lived experiences of mental health conditions. Yet, mental health still occupies a miniscule share (0.06 percent) of budgetary allocations to health in India, reflective of global budgetary trends (under two percent). The reluctance to appropriately budget for mental health stems partly from a failure to see mental health as a development issue, and an inability to join the dots between mental health and social conditions of poverty.
Mental illness and poverty are intricate parts of a vicious cycle.
We intuitively understand that living on the streets, being unemployed for extended periods, not knowing where one’s next meal is coming from, the constant threat of eviction or violence, or social exclusion on account of caste, gender, or sexual identity, would distress anyone. Mental distress in turn impacts the ability to hold a job or complete education, inhibits participation in social and family activities, decreases productivity, and diminishes resources within families. It isn’t surprising then, that those living with mental health conditions might simultaneously grapple with unemployment, low education, food insecurity, inadequate housing, and financial stress. Mental illness and poverty are thus intricate parts of a vicious cycle: poverty increases the risk of mental health conditions and conversely, those living with mental health conditions are more likely to drift into poverty.
Related article: Mental health in India: Underserved and underfunded
Within this self-fortifying cycle of mental illness and poverty, certain groups emerge more vulnerable than others. Social hierarchies—of gender, sexual orientation, economic status, ability, and caste—exclude, discriminate against, marginalise, and isolate certain groups and individuals. Consequently, we find that marginalised groups that hold lower positions within these social hierarchies experience greater levels of mental distress than those who hold more advantaged or higher positions.
According to data from the National Crime Records Bureau, 2014, people from Scheduled Tribes had the highest suicide rate 1 at 10.4, followed by Dalits at 9.4. In less than a decade, more than 25 Dalit students in India have died by suicide due to caste discrimination and institutional casteism in educational institutions such as University of Hyderabad, AIIMS, and IIT. The Banyan—a Chennai-based mental health organisation that provides comprehensive services for people with mental illness living in poverty and homelessness—noted through their research that one in every three homeless individuals suffers from a mental illness. Similarly, LGBTQIA+ individuals face unique life stressors such as familial violence, discrimination, and violence in public spaces and institutions, contributing to a significant impact on their mental health. The global suicide rate among trans or non-binary gender persons ranges from 32 to 50 percent, significantly higher than the average global suicide rate.
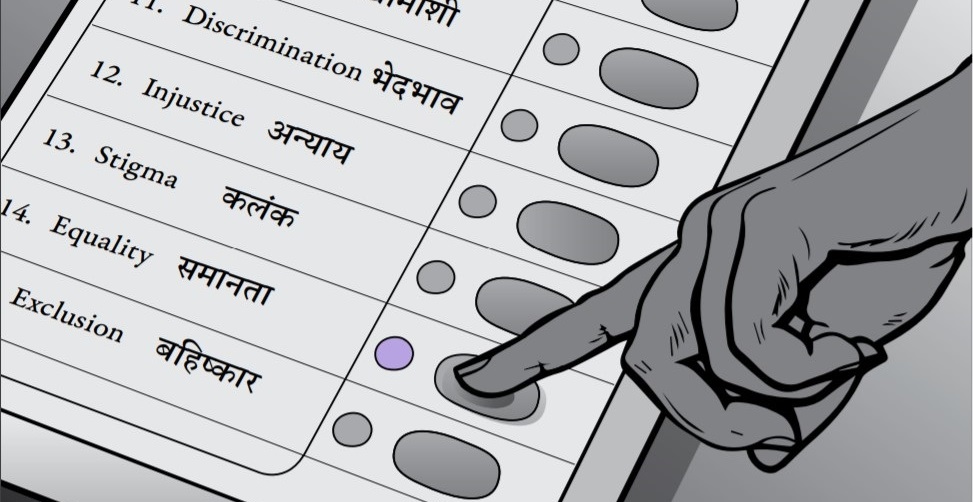
Social hierarchies—of gender, sexual orientation, economic status, ability, and caste—exclude, discriminate against, marginalise, and isolate certain groups and individuals. | Photo courtesy: ReFrame Issue No. 2/Studio Kohl
We are surrounded by such examples of how mental health coexists with social, economic, and environmental conditions. In fact, mental health cuts across and influences several Sustainable Development Goals (SDGs)—all of which will remain unattainable unless mental health is integrated into development programmes. For instance, let’s take SDG-3: Ensure healthy lives and promote well-being for all at all ages. There is a high level of comorbidity between mental illness and physical illness that underlines why health services need to be provided in an integrated manner.
For example, maternal depression has been shown to increase the risk of poor infant nutrition, stunting, and diarrheal disease. If we want to influence better health outcomes for infants, we must ensure that pregnant women or mothers of infants are routinely screened for mental health conditions and provided with appropriate care and treatment. Similarly, depression has been shown to adversely affect adherence to antiretroviral medication among those living with HIV/AIDS. Again, to influence better health outcomes, mental health care and treatment should be integrated within HIV/AIDS programmes.
Mental health clearly cannot be addressed in isolation. The WHO’s Comprehensive Mental Health Action Plan (2013–2020) advocates for ‘mainstreaming mental health interventions into health, poverty reduction, development policies, strategies and interventions’. Fostering linkages between mental health service providers and allied service providers—for livelihoods, health, education, legal support, and government welfare schemes—is important. At Mariwala Health Initiative (MHI), one way in which we facilitate this, is through a school-based mental health justice programme that addresses psychosocial distress within the education system. This is especially pertinent among vulnerable communities that face mental distress due to multiple axes of marginalisation. This programme aims to better equip educational spaces to enhance mental well-being among marginalised and vulnerable youth.
We need to take a closer look at how the intersections of poverty, casteism, misogyny, and other forms of violence impact mental health.
Another example of integrating mental health within development programs is our disaster-related psychosocial programme. Despite evidence of the impact that disasters have on mental health, disaster response approaches traditionally have not included mental health services, and tend to focus solely on immediate humanitarian needs (protection, water, sanitation, shelter, food, and health).
Related article: Changing the way we think about mental health
Consequently, while disaster-related distress is highly prevalent in affected communities, those experiencing such distress usually have no recourse. If we were to integrate mental health within a disaster-response programme, we would, for instance, consider how overcrowding and lack of privacy and safety in disaster relief camps increases distress for vulnerable groups such as women and children. We would draw on a community’s inherent resources—which might include the ways in which people have dealt with adversity previously, and traditional solidarities that provide mutual support. In situations of disaster, these networks and mechanisms for psychosocial wellbeing and mental health may face undue strain or break down, making it even more imperative to revive them.
These examples of how mental health can be integrated within education and disaster-response programmes hold true for other sectors as well. We need to locate mental health within economic, environmental, sociocultural, and political contexts. We also need to take a closer at how the intersections of poverty, casteism, misogyny, and other forms of violence impact mental health, and include it as a key ingredient across development programmes.
- Suicide rate refers to the number of suicides per population of one lakh.
—
Know more
- Learn more about mental health and mental illness.
- Read this article to learn about how Indians perceive mental health.
- Dip into resources from the Mental Health Innovation Network, a global community of mental health innovators.
Do more
- Explore Mental Health Matters to learn how to incorporate a mental health component into your existing development program.