The COVID-19 pandemic has swept the world since 2020, causing over 5 lakh deaths in India alone, necessitating us to look at the country’s capacity to combat infectious diseases, specifically, the world’s second-largest killer among infectious diseases, tuberculosis.
Over 3 lakh people died in 2021 due to the coronavirus during the disastrous second wave of the pandemic. Comparatively, in 2020 alone, approximately 5 lakh people died due to Tuberculosis (TB) in India, a preventable disease that has been prevalent in the country for centuries now.
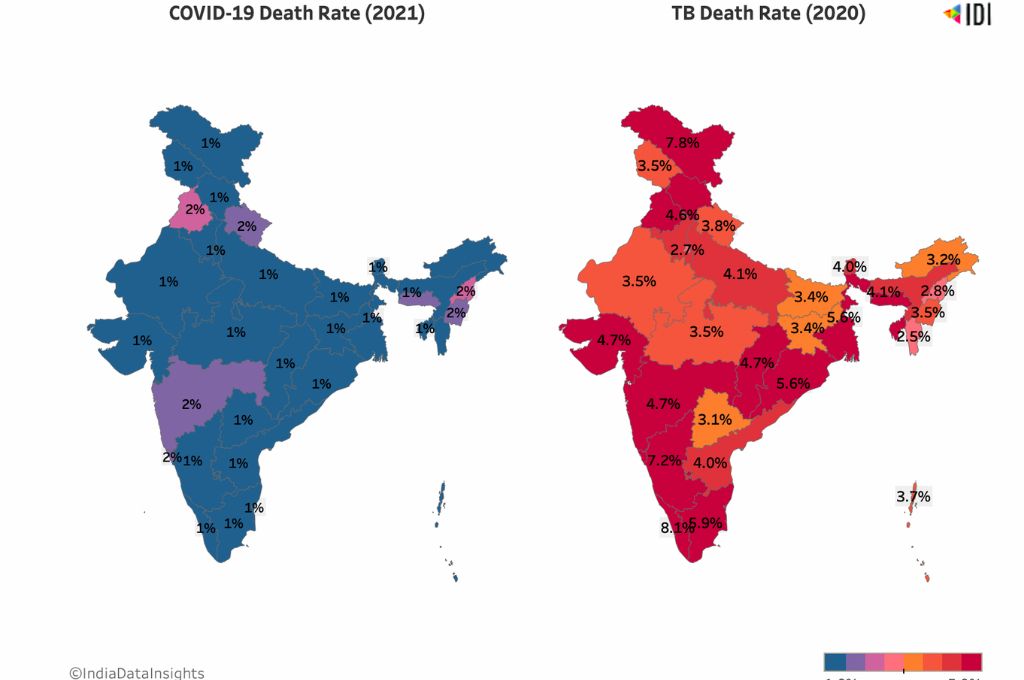
India has set a mammoth task of eliminating TB by 2025. With only three years left to achieve this goal, it has become more ambitious as the pandemic has regressed years’ worth of efforts for TB—from testing to treatment.
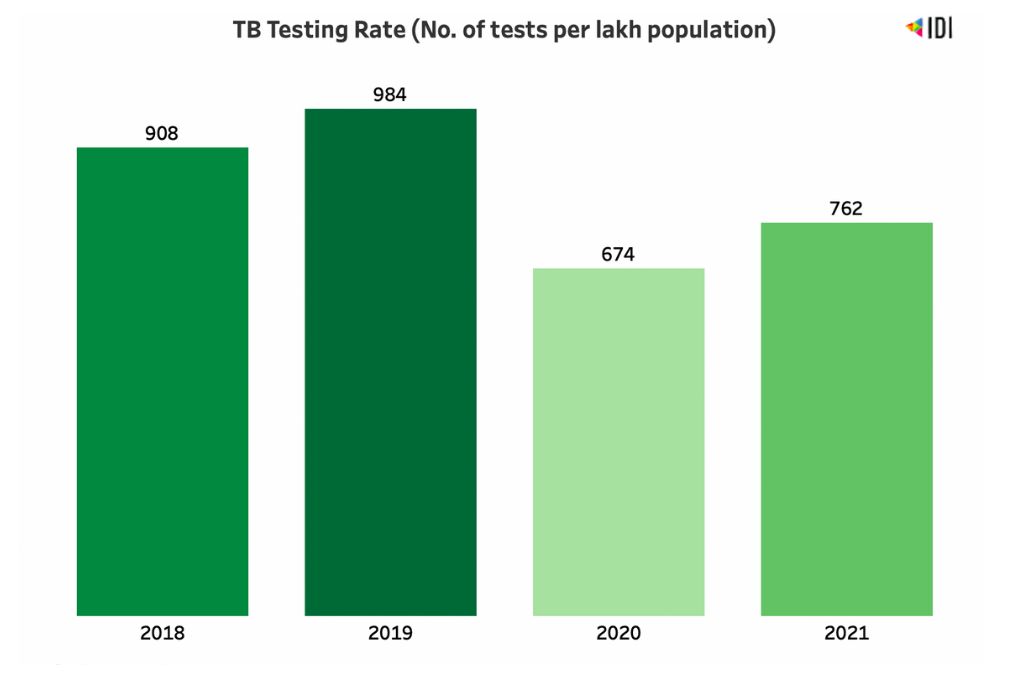
TB tests had dropped by more than 30% across the nation in 2020 due to lockdowns and containment measures. In 2021 however, we saw a 13% rise in tests from 2020, but still 23% less than the pre-pandemic testing rate in 2019.
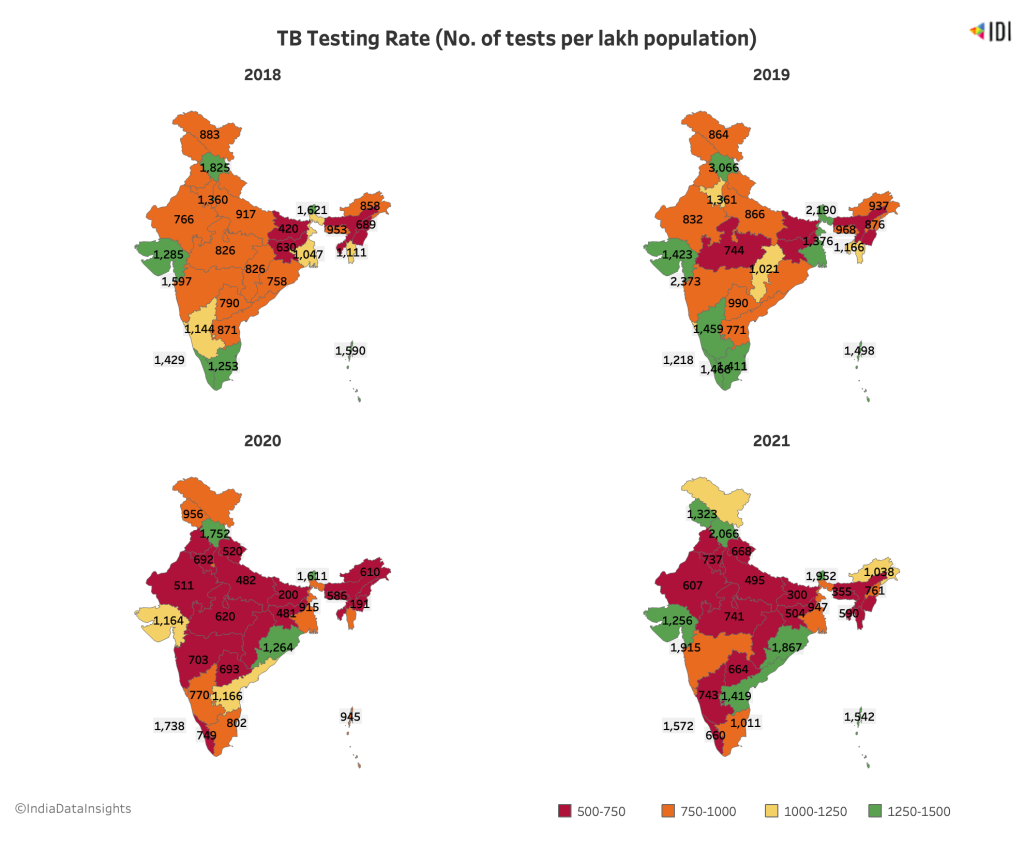
Across the country, testing for TB has dropped by a significant amount since the onset of the pandemic. The southern states, which had higher pre-pandemic testing, now fare poorly (except for Andhra Pradesh), while Bihar, Uttar Pradesh and Jharkhand have had the worst testing rate.
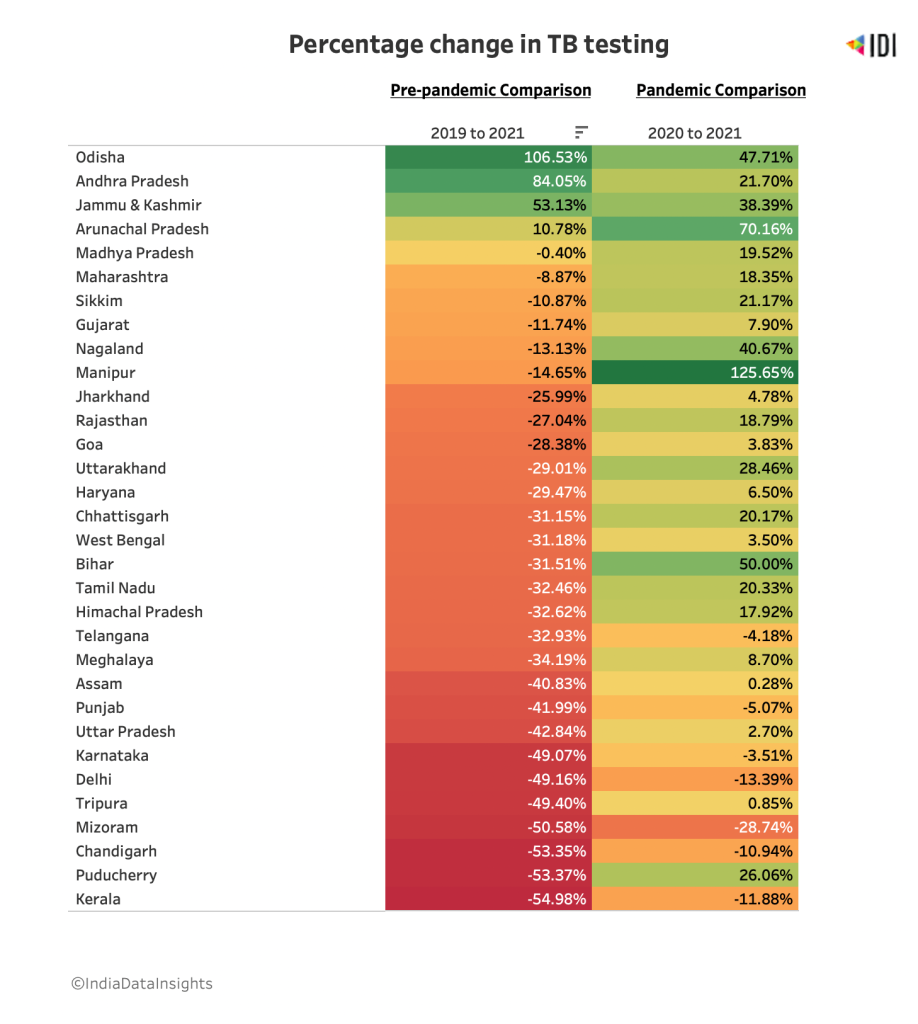
Interestingly, Odisha has witnessed a doubling in TB testing since the onset of the pandemic. Only three other states have shown a continued increase in testing in line with the TB elimination targets despite the increased burden on the health systems—Andhra Pradesh, Jammu & Kashmir and Arunachal Pradesh. States such as Manipur and Bihar made strides in 2021 after a steep fall in tests in 2020.
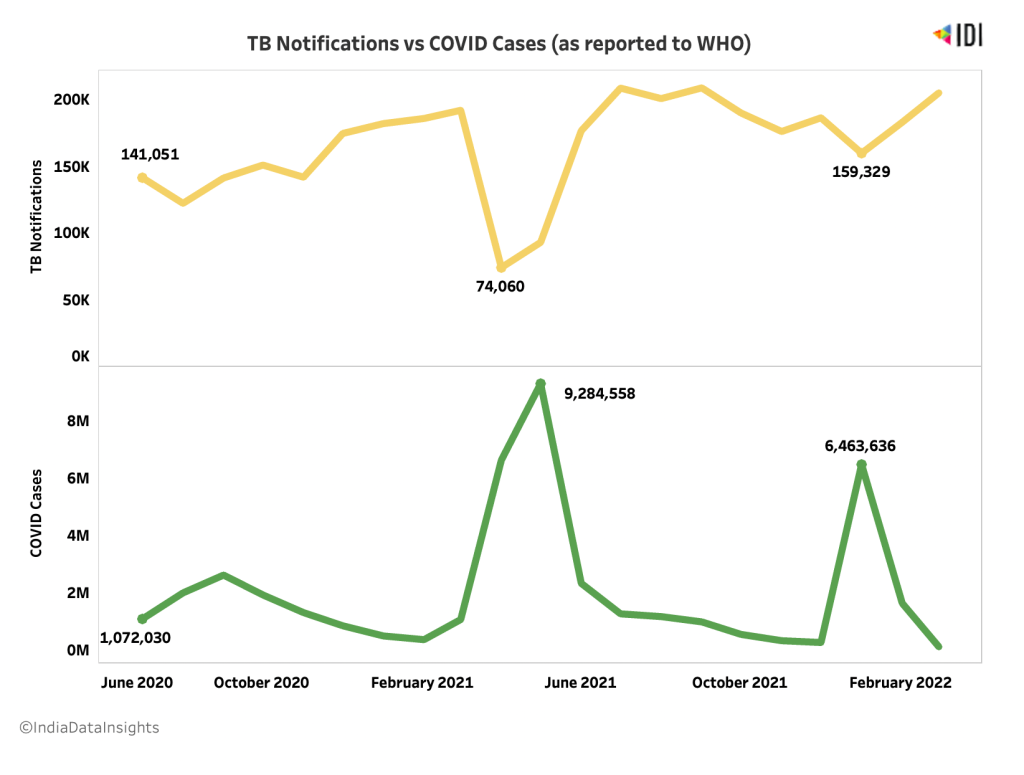
We see a steep decline in TB notifications during the second wave of COVID-19, in line with the worsening of the pandemic, indicating poorer testing and reporting of TB cases. TB notifications mean that TB is diagnosed in a patient and reported within the national surveillance system and then to WHO. Incidentally, when we see a dip in COVID cases post wave 2, we see a rise in TB notifications.
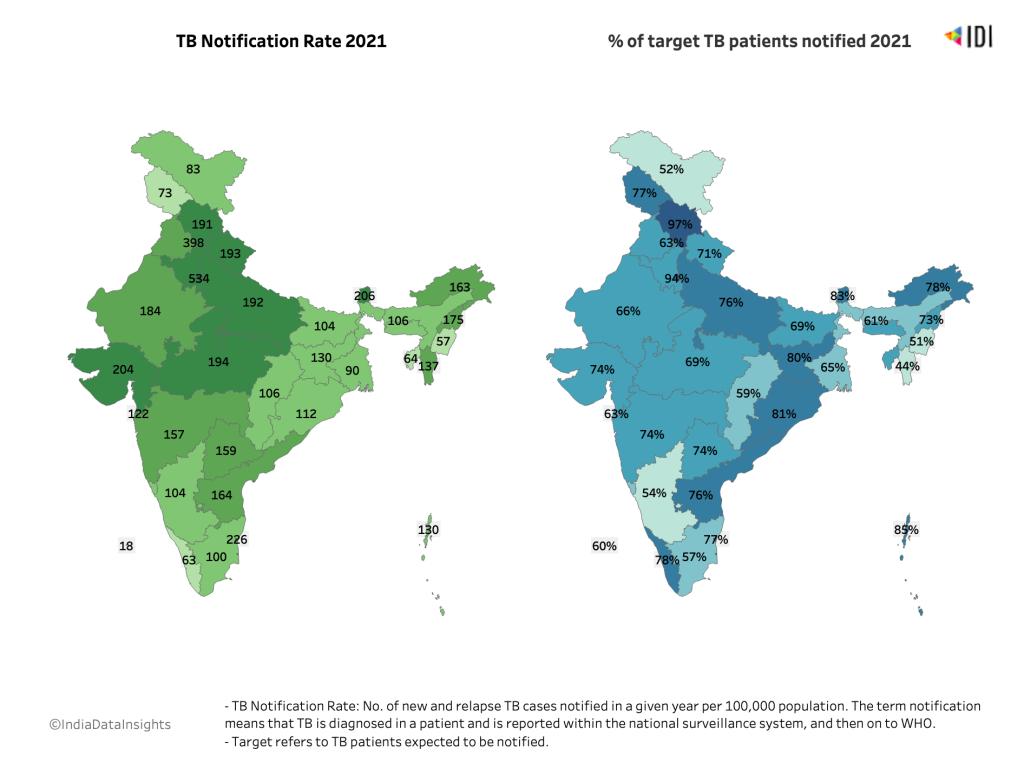
The sudden decrease in notifications has concerned authorities not as a decrease in TB cases but as possible indicators of poorer testing. Among various infectious diseases, TB has a high mortality risk of 4%. Globally, this translates to 1.5 million deaths a year (for comparison, the coronavirus has claimed 6 million lives so far).
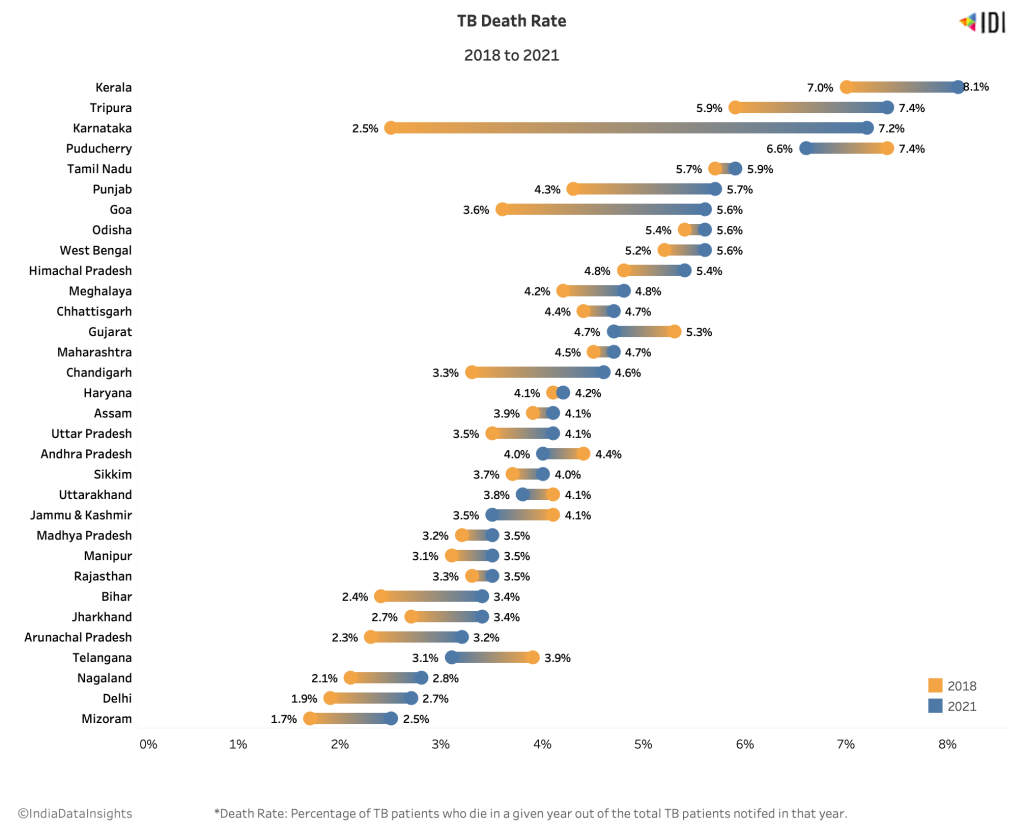
While the death rate has remained the same from 2017 to 2019, we see a steep rise in deaths in 2018, with a simultaneous increase in TB cases and a subsequent drop. Karnataka stands out in the steep rise in the death rate from 2.5% in 2020 to 7% in 2021. Gujarat, Andhra Pradesh and Jammu & Kashmir are the only three states that show a fall in the death rate from 2020 to 2021.
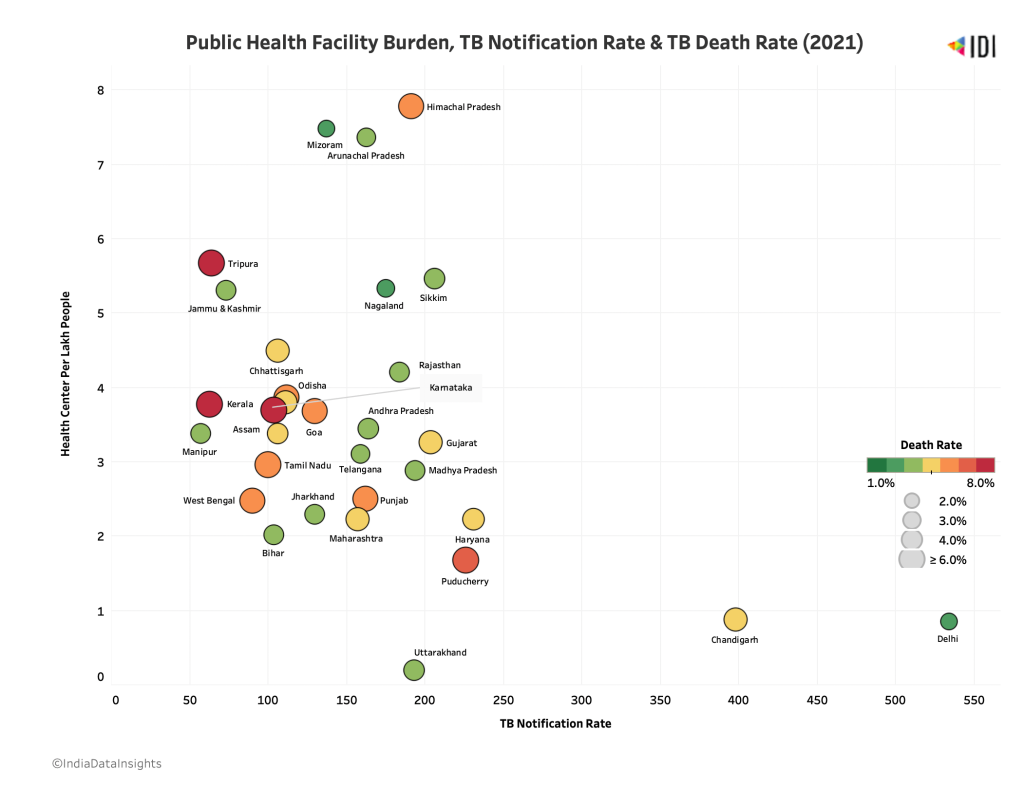
The pandemic has brought to light the state of health infrastructure in the country and has catalysed our efforts for healthcare system strengthening. The scatter plot shows the varied relationship between TB notification rates, death rates, and health facility burden. States such as Tripura report good health facilities yet show high deaths and cases. On the other hand, states such as Himachal Pradesh report high deaths despite good facilities. Bihar reports both low death rates and low notification rates. Overall, the dispersion of the scatterplot indicates the distinct challenges that each state proposes.
Treatment of TB is multifold, along with a fixed-dose combination of drugs for months; diet and nutrition play an essential role in treating the disease. To this end, nutritional support becomes a necessary part of TB treatment, especially among the poor. In addition, TB often leads to loss of livelihood and added expenses of diet and treatment, making financial assistance a necessity.
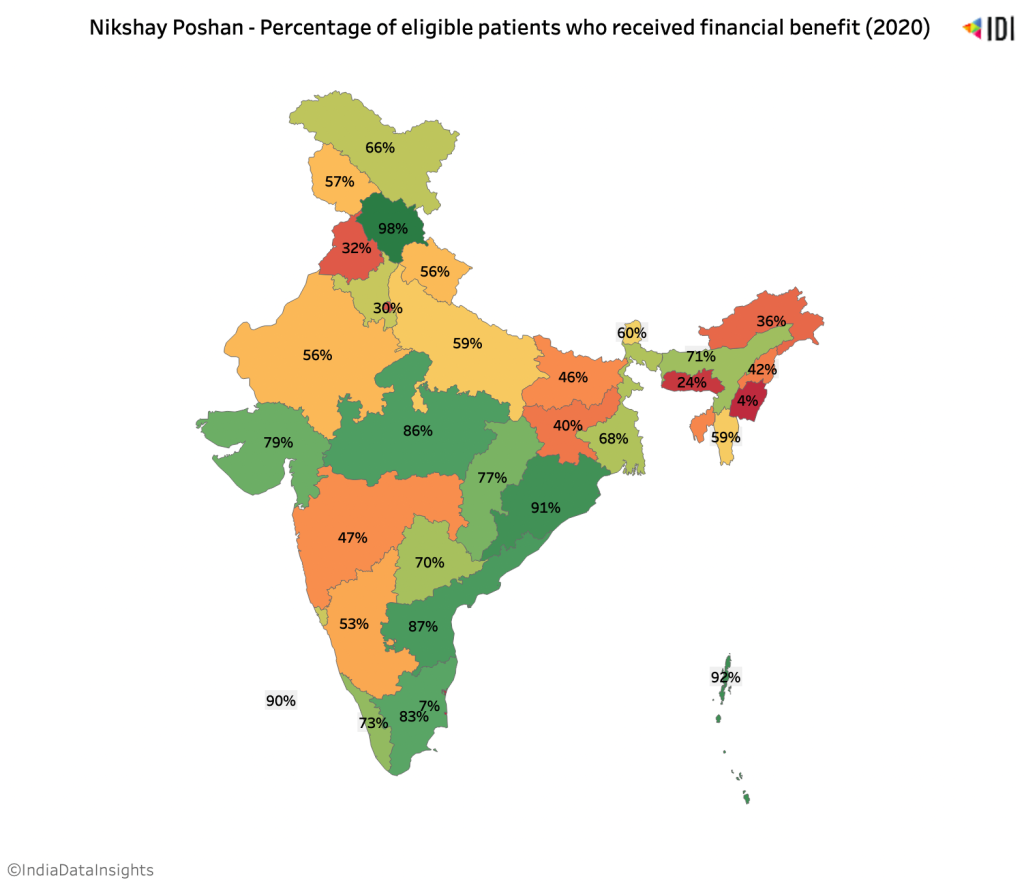
The government has thereby rolled out Nikshay Poshan Yojana, a scheme to provide nutritional support to TB patients. All notified TB patients are to receive 500 rupees in cash or in kind. On average, 62% of the notified patients in the country received the benefit in 2021.
While a large proportion of beneficiaries receive nutritional support in states such as Andhra Pradesh and Himachal Pradesh, states such as Delhi, Meghalaya and Manipur lag far behind. According to the Central TB Division, one of the main reasons for the variation seen across the country is the non-availability of bank accounts and unlinked bank accounts, making direct benefit transfers difficult.
The flatlining of philanthropic funds also raises huge concerns. Funding for COVID in the span of 2 years has been exponentially higher than what has been catered to TB research and medication over many years. To add to the woes of poor financing, drug-resistant TB—where bacteria become resistant to the drugs used to treat TB—has been on the rise.
While the situation looks grim, the pandemic could also be a vehicle to strengthen the healthcare system and funding. For example, during the pandemic, there has been a ramp-up of various molecular diagnostic tools for TB and an attempt to implement bidirectional screening for COVID-19. The pandemic has thereby laid the ground for improved surveillance methodologies, which, when combined with a considerable increase in funding and 100% implementation of benefit schemes, could pave the way for TB eradication.
This article was originally published on India Data Insights.
—
Know more
- Sign up to India Data Insights to access more tuberculosis-related data in the Indian context.
- Write to idi@sattva.co.in to know more about tuberculosis prevention and cure efforts.





