Just over 20 percent of India’s adult population has received their first COVID-19 vaccine dose. During the rollout, clear gender disparities have emerged, and these are of concern for the coming months. In a recent map released by Ashoka University, only around 86 women are receiving vaccine doses for every 100 men. According to data from the government’s CoWIN dashboard, in only three states—Chhattisgarh, Himachal Pradesh, and Kerala—are women currently receiving an equal or higher number of vaccine shots compared to men. Union territories including Dadra and Nagar Haveli, Daman and Diu, Jammu and Kashmir, and Chandigarh are the worst-performing regions on vaccine gender parity. As the vaccination programme begins in rural areas, addressing this gender gap early is a priority.
In the initial days of the vaccine rollout, women made up the majority of vaccine recipients given that many frontline jobs are performed by women. In March 2021, when vaccines became available to those over 45 years of age, and then in May 2021 to those between ages 18 to 44 years, the numbers began reversing, with more men being vaccinated than women. In April alone, 2.4 million fewer women than men received a vaccination.
How did we get here?
Although often unacknowledged, a primary barrier to getting women vaccinated is the limited understanding of the disparate physical impacts COVID-19 and vaccines have on women’s bodies. Out of those who contract the virus, men are typically sicker and die at higher rates, while women are more likely to have long-term effects, or ‘long COVID-19’ (particularly with the Delta strain). And while there are very few trials available that capture the sex-differentiated impacts of different COVID-19 vaccines, those that do exist suggest that although women have a stronger immune response that aids vaccine efficacy, they also experience more frequent and severe adverse effects post-injection.
The opening of online registrations (in English only) for those aged 18-44 in March 2021, ignored the historic digital divide between men and women.
There are also many misconceptions regarding the effects of the vaccine. In a recent study by the Self-Employed Women’s Association (SEWA), poor women spoke candidly about how the vaccine might inject a virus into them and put them out of work for a few days. There are also concerns around the vaccine affecting pregnant women, menstrual cycles, and fertility rates. Many public health researchers rue the lack of sufficient clinical trials around the COVID-19 vaccines for not being able to pass on accurate information about the after-effects of the vaccine, especially on women.
For women seeking to get vaccinated, securing a vaccine dose is complicated by existing gender inequities in society. For example, rural women face technological barriers in registering for a shot. The opening of online registrations (in English only) for those aged 18-44 in March 2021, ignored the historic digital divide between men and women. This gap is most prominent in rural areas, where according to data released by the fifth round of the National Family Health Survey (NFHS), only 33.9 percent of women have ever used the internet compared to 55.6 percent of men and only 54.8 percent own a personal mobile phone, with far fewer owning a smartphone. The government has recently tried to rectify this gap by allowing walk-in vaccinations and registrations in Hindi.
Many women also hesitate to take vaccines because of mobility issues, having to rely on some male family member to accompany them. For mothers, travelling long distances to health clinics may not be possible with unattended children at home. Religious practices or cultural values may prevent some women from seeking immunisation services from male health workers. In the current pandemic, health workers are also realising how difficult it is to bring elderly women to wait in long queues at vaccination centres.
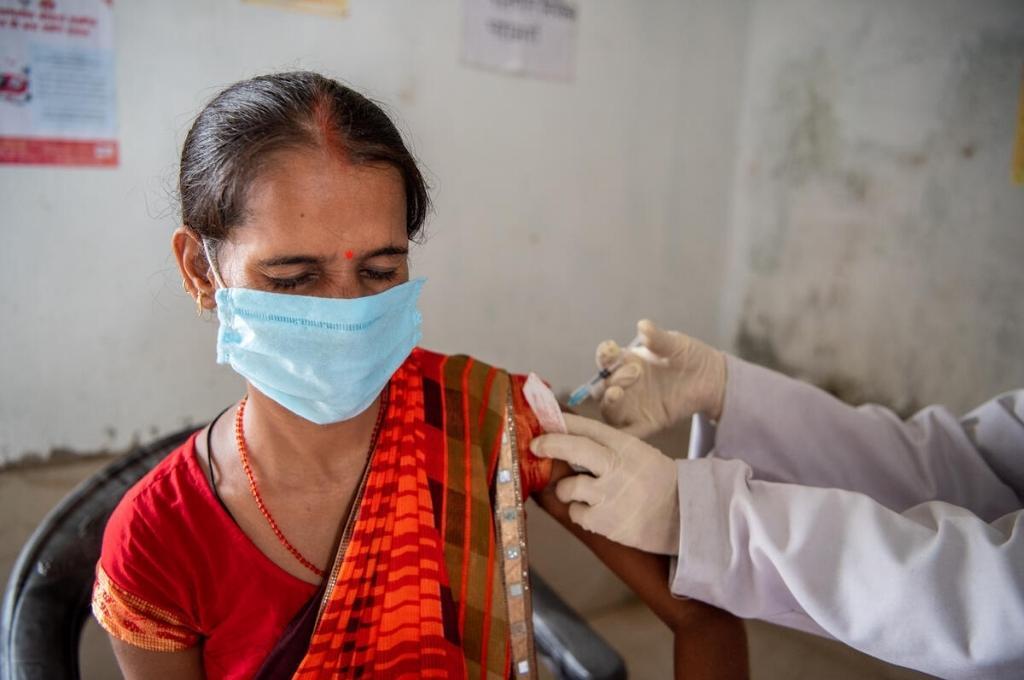
India’s history of vaccine disparity
Prior studies around immunisation programmes in India, including child immunisation programmes, show gender gaps. A study conducted by A Singh used NFHS data to track immunisation rates for male and female siblings within the same household. It found that immunisation completion for girls is lower than for boys. Since the comparison is between children in the same household, the author concludes that the gap cannot be explained by household-level factors that drive immunisation (eg. poverty or access); instead, it could be explained by intra-household inequality between girls and boys. Unfortunately, as of July 5, 2021, we do not have data on intra-household vaccine completion for COVID-19.
Gender inequality is worsening the COVID-19 vaccine gap
Ongoing analysis by IWWAGE is beginning to explore the connections between these larger gender inequalities in society and gender disparities in COVID-19 vaccinations. Using data from the government’s CoWIN dashboard, we are finding that states with a higher percentage of females being vaccinated are also likely to have lower poverty levels, higher female education levels, and a higher share of women reporting intra-household bargaining power. Generally speaking, our findings suggest that states performing better on gender outcomes are more likely to have higher female vaccination rates.
The more women that are working, the better their vaccination rates, and vice versa.
Specifically, two indicators stand out. First, women’s employment: The share of vaccinated women is positively correlated with women’s labour force participation rates, and negatively with the share of women not working due to domestic duties and care work. In other words, the more women that are working, the better their vaccination rates, and vice versa. Second, women’s local-level political involvement in Panchayati Raj institutions strongly matters too. These findings echo previous evidence on the role of women’s political leadership in the improved provision of public services and redressal of women’s issues.
So what can be done?
India needs a more holistic, gender-sensitive vaccine rollout strategy. The following are some suggestions to achieve this:
- First, vaccine delivery must account for women’s barriers—of access, information, and mobility—that prevent them from getting vaccinated. Greater engagement with community organisations in planning, targeting, and communicating with women on the ground can be tremendously impactful in identifying barriers, building trust, and dispelling misinformation.
- Second, vaccine delivery should be planned based on context-specific needs and preferences of women, addressing mobility and digital barriers.
- Third, India needs to rely on its overstretched female frontline staff to ensure the vaccine’s social acceptability in communities. But to do so, it must ensure that they themselves are vaccinated, remunerated on time, and receive adequate training.
- Fourth, vaccine data systems should collect data on the gender of those vaccinated in order to be able to identify gaps and better target those in need. In the current CoWIN dashboard, gender has not been reported for nearly 20 percent of those vaccinated until May 2021. If one were to exclude this population, the share of women receiving the COVID-19 vaccinations dips even further to 74 women per 100 men receiving their vaccine shots.
- Fifth, and above all, we need to recognise the relationship between the current state of gender equality and the vaccine rollout, and understand that improving gender equality on other fronts can improve gender-balanced vaccine efforts. Without this, women will continue to face a disproportionate burden of the COVID-19 pandemic.
—
Know more
- Understand why it is imporant to take notice of the gender gap in vaccination.
- Learn more about why clinical trials don’t report gender data despite COVID-19 affecting men and women differently.






