“I work at a tiffin centre so that I can bring home leftovers to feed the kids.”
“We sold our livestock to buy foodgrains.”
“We eat just once a day and give our share of food to our two children.”
At Cuddles Foundation, we constantly hear variations of this theme from the families and caregivers of children fighting cancer. Nutrition plays an important supportive role in cancer treatment, and therefore it is important to understand the extent and impact of food insecurity in childhood cancer patients.
What is food insecurity and how does it affect health outcomes?
Johns Hopkins University classifies food insecurity as a state when one cannot consistently afford healthy or adequate food. The Food and Agriculture Organization (FAO) estimated that in 2021 approximately 2.3 billion people—which is 29.3 percent of the world’s population—suffered from food insecurity. Closer to home, the 2022 Global Hunger Index Report ranked India 107 out of 121 countries, and noted its high burden of poverty, food insecurity, and malnutrition.
As of 2022, India accounts for nearly a quarter of all undernourished people worldwide. With malnutrition in India being well above acceptable levels and large numbers of women and children suffering from micronutrient deficiency disorders, there is a high risk that public health will be affected directly and indirectly.
In food-insecure households, the need for other basic human necessities such as housing, medication, transportation, and utilities often competes with the need for food. Spending on nutritious and quality foods such as pulses, fruits, and fresh vegetables is difficult when budgets are stretched, and households opt for cheaper, less nutritious alternatives. This often compromises both the quality and the quantity of the food being consumed, leading to an increased risk of malnutrition. In these situations, malnutrition becomes a serious problem that can significantly contribute to morbidity and mortality, specifically among children under five.
On the other hand, in a food-secure household, adequate quantity and quality of food can protect its members against nutritional deficiencies and may help prevent or delay the onset of non-communicable diseases such as diabetes, hypertension, and cardiac ailments.
Food insecurity in children with cancer
Malnutrition due to inadequate food supply caused by economic, social, and environmental factors is termed primary acute malnutrition and manifests as wasting in children. This results in them being too thin and having a weakened immune system and makes them vulnerable to developmental delays, disease, and even death. In the event of illnesses, children living in food-insecure households may experience higher hospitalisation rates and longer recovery periods.
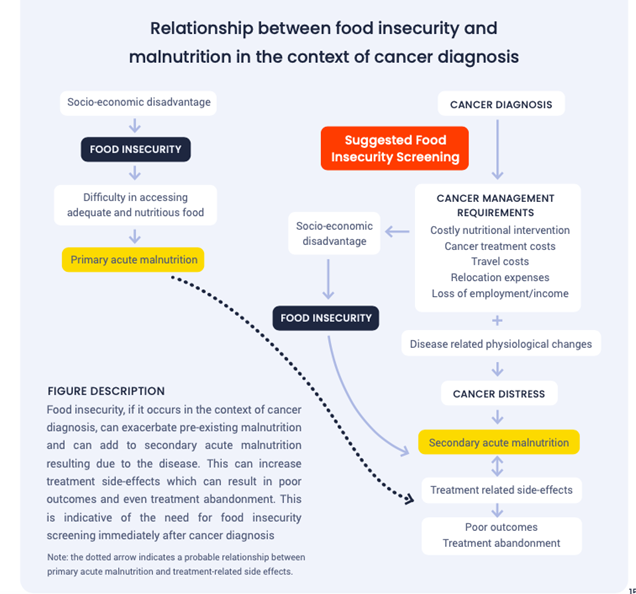
Annually in India, it is estimated that approximately 76,000 children may develop cancer, and nutrition plays a crucial role in their recovery. Well-nourished children have better tolerance to treatment, fewer side effects and infections, and lesser treatment delays. Food insecurity, on the other hand, may have a catastrophic impact on the entire cancer care process, derailing treatment adherence and completion. For instance, if a child does not have access to adequate nutrition, their capacity to overcome treatment side effects such as vomiting, diarrhoea, and mouth sores is heavily reduced.
Malnutrition in children diagnosed with cancer is very common, especially in lower-middle-income countries like India. It is estimated that approximately 40 percent of children with cancer are already malnourished at the time of diagnosis. Cancer therapy can further worsen a child’s nutritional status and result in secondary acute malnutrition. This form of malnutrition, marked by loss of muscle and body fat, is due to the metabolic changes that the disease and its treatment causes. In this context, it is essential to ascertain potential levels of food insecurity among patients with childhood cancer in order to address their nutrition needs effectively.
In 2021, we at Cuddles Foundation conducted an internal study to better understand the socio-economic status of the communities we work with. This study covered a total of 1,105 children across 34 partner hospitals. The results showed that 51.4 percent of households surveyed earned INR 10,001 per month or less, 31.8 percent earned between INR 10,002 and INR 29,972, and 11.8 percent earned between INR 29,973 and INR 49,961.
Since food insecurity is often linked to socio-economic disadvantage, we further investigated the prevalence of food insecurity among the communities we work with. The results indicated that a majority (82 percent) of the children that we supported had been at risk of being food insecure the year before they were initiated into our programme, that is, even before their cancer diagnosis.
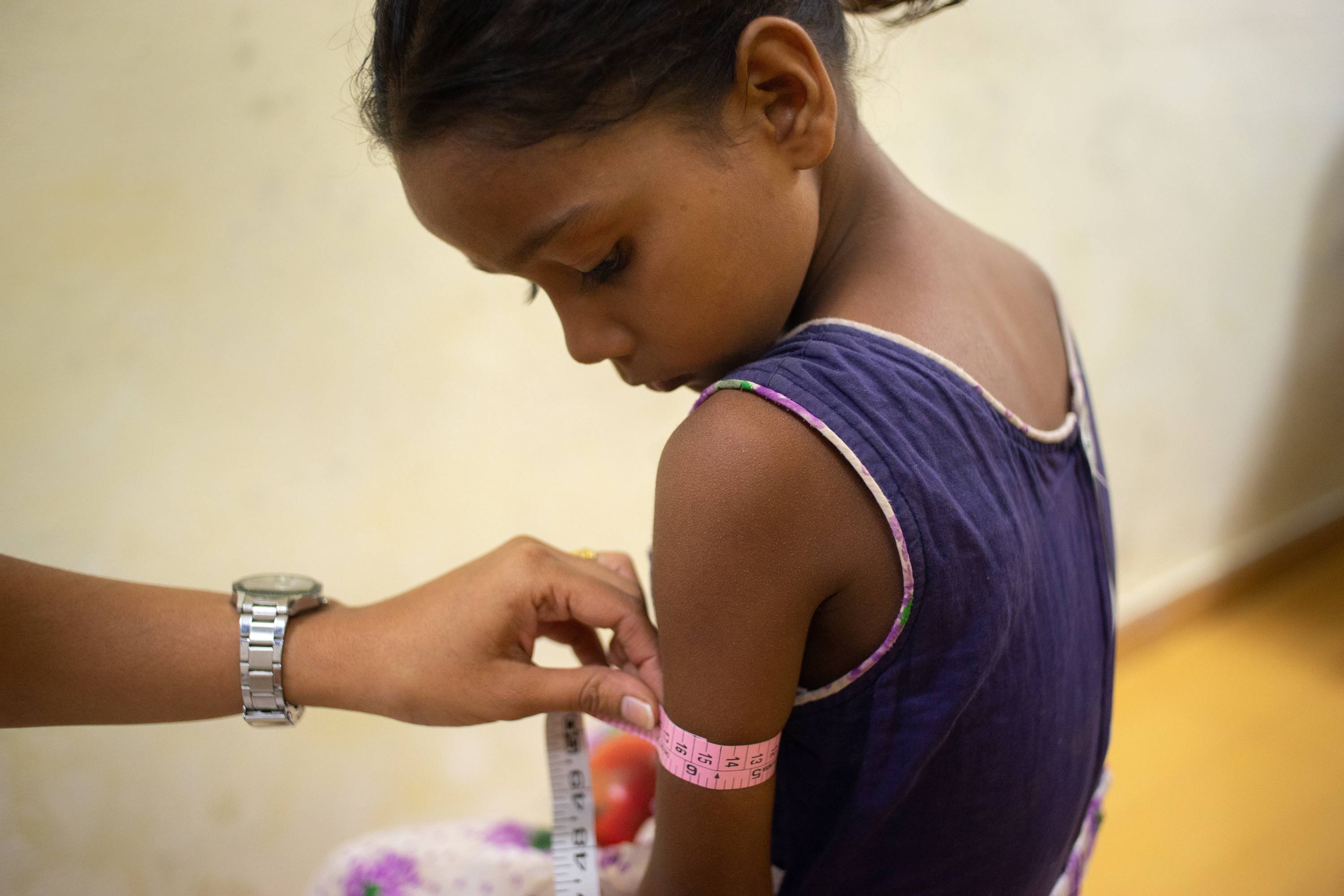
Improving food security for children with cancer
Cancer care centres can play an important role in ensuring that the nutritional needs of children with cancer are being met.
1. Conducting screenings early on
Given the robust association connecting food insecurity with poor health outcomes, organisations such as the American Academy of Pediatrics and the American Diabetes Association have advocated for the regular screening of patients for food insecurity in clinical settings. The American Cancer Society has also called for the need to make food insecurity assessments a necessary tool in the treatment of cancer. This is important because response to cancer treatment is dependent upon nutritional status, and assessing levels of food insecurity in patients and caregivers (specifically the economically disadvantaged) could determine the trajectory of care as well as recovery.
Cancer care centres should ideally incorporate food insecurity screening during the patient’s initial visit. To determine cancer care requirements during treatment, paediatric cancer units already deploy various assessments to cover socio-economic, demographic, and nutritional backgrounds of patients. Along with this background screening, simple questionnaire-based surveys and scales can be used to measure food insecurity.1
We assessed food insecurity using the The Hunger Vital Sign tool, which is the most common screening tool in the US and can be used with both adults and children. The tool helps identify households at risk of food insecurity if their answer to either one or both of the survey’s statements is ‘often true’ or ‘sometimes true’ (as opposed to ‘never true’). The two statements in the survey are:
- “Within the past 12 months we worried whether our food would run out before we got money to buy more.”
- “Within the past 12 months the food we bought just didn’t last and we didn’t have money to get more.”
Employing such screening tools can enable holistic care for children with cancer and help them become more tolerant to treatment and treatment outcomes.
2. Regularly monitoring nutritional deficiencies
Constant monitoring and correction of nutritional deficiencies during the time of diagnosis and throughout the treatment can minimise the side effects of treatment, improve chances of survival, and reduce the risk of nutritional morbidity.
3. Building awareness about food insecurity and cancer
An internal study indicated that 80.1 percent of caregivers did not know the proper foods to feed their child when they were diagnosed with cancer. It is therefore important to create specific educational initiatives to sensitise caregivers on the complex relationship between food insecurity, malnutrition, and treatment outcomes.
4. Linking families to assistance programmes
Screening centres can facilitate and help link eligible families with governmental and non-governmental food assistance programmes within the earliest possible time frame. Some of the governmental food assistance programmes under the National Food Security Act, 2013, include ONORC (One Nation One Ration Card), the Poshan Abhiyaan scheme, and the Midday Meal scheme.
Food insecurity is a human developmental challenge that has an immense impact on health outcomes. In particular, in the context of children with cancer in India, pre-existing food insecurity and resulting malnutrition may compromise their odds of survival as they are more prone to risks of infection and treatment-related toxicities. Implementing food insecurity screening will enable a system where all children with cancer can be connected to resources that may help provide regular and timely access to enough nutritious food. The ability to access healthy and adequate food may result in improved treatment outcomes.
—
Footnotes:
- Two popular tools used in assessing food insecurity are The US Household Food Security Survey Module and The Food Insecurity Experience Scale.
—
Know more:
- Explore the latest report by Cuddles Foundation to learn more about the link between food insecurity and childhood cancer management.
- Read this article to understand why food insecurity in India is not a scarcity problem, but a distribution problem.
- Learn more about the impact of climate change on India’s food security.