I am an Urdu desktop publisher and have been working with Pratham for more than eleven years now. Before COVID-19 happened, my work primarily involved creating educational material—both print and digital—which would then be used to teach children from marginalised communities in Mumbai.
When the pandemic hit Mumbai, Antop Hill where I stay—which is part of Mumbai’s F-North ward—was selected along with two other wards (Chembur’s MW ward, Dahisar’s RN ward) for the sero survey conducted by the Municipal Corporation of Greater Mumbai (MCGM). The first round was conducted between 29th June, 2020 and 13th July, 2020 in our ward and I was picked to be part of this process.
A sero survey involves testing the blood serum of a group of individuals to monitor trends in prevalence of COVID-19 infection at the district level. It was conducted by Tata Institute of Fundamental Research (TIFR), MCGM, NITI Aayog and other partners in collaboration with key stakeholders and state health departments.
We didn’t know what a sero survey was; we hadn’t even heard of it. Once selected though, I was part of continuous Zoom calls where we were told about the survey strategy, how it had to be executed on the ground, who would be part of the team, what our roles would be, and so on.
A team of 36 people was eventually put together for our ward. It comprised of 12 nonprofit volunteers (in our case, most were employees of Pratham), 12 community health workers (CHWs) from MCGM, and 12 lab technicians from Thyrocare—the organisation in charge of collecting the blood samples for antibody testing. I was appointed the field manager for the entire team.
The pre-survey planning was detailed and rigorous.
The pre-survey planning was detailed and rigorous. Fourteen communities in our ward were identified and their locations were shared using Google Maps. We were given a target for each community based on the population of the area—for instance, we had a target of 500 people for Sangam Nagar. We then coordinated with MCGM’s Medical Health Officers (MHOs), since we had to work with them to administer the survey in their wards. This joint planning would entail finalising the location for the next day, the target for each community, the number of people who would accompany us, and other operational details.
We set up camps in each community for two days at a time. Each day’s collection was different, ranging from around 100-200 samples, based on the community’s response. We also had to decide which language forms to give, where for instance, in localities with a predominantly Muslim population we gave out the consent forms in Hindi; and in areas like Ganeshnagar and Shantinagar, we used Marathi forms.
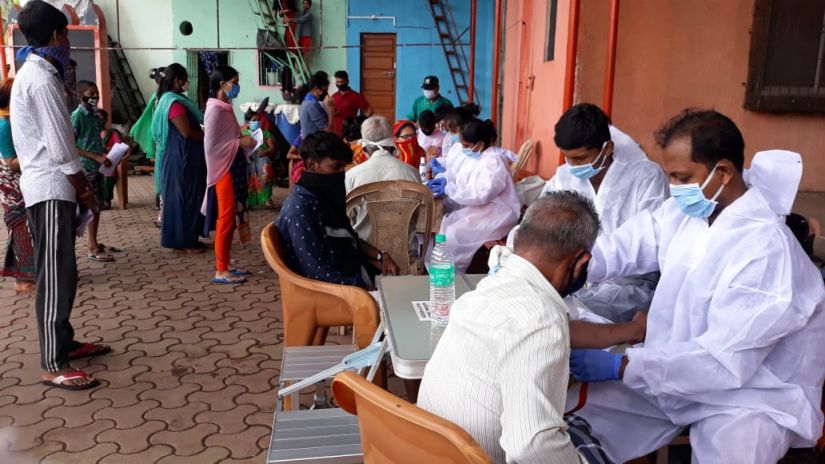
“We set up camps in each community for two days at a time. Each day’s collection was different, ranging from around 100-200 samples, based on the community’s response.” | Picture courtesy: Naziya Faiz Shaikh
6.30 AM: I start getting calls from volunteers for directions to the day’s meeting point. This is usually an MCGM health post located within the community. The location is decided the night before, after consulting various stakeholders of the survey.
9 AM: We all arrive at the predetermined meeting point. From here, pairs comprising a CHW and a Pratham volunteer start preparing to set out to meet the identified communities for the day.
There are two camps set up for each location, and the 36 member team is evenly split between them. These camps are typically set up near the local temple or madrasas—places that people are familiar with and have no trouble locating. At other times, we set up camps in the offices of the local corporators. In a couple of instances where there were no nearby structures, we sat under the open sun.
While CHWs are aware of the conditions within certain localities—in some instances the camps are in congested, not-so-clean locations—we’ve had to spend time placating and convincing the larger team to adjust with the surroundings. Access to, and the use of washrooms is also a big challenge.
10 AM: The CHWs and Pratham volunteers go door-to-door to talk to people in their homes. They get people to fill up and sign on consent forms. We have been trained to select every fourth house for the survey—the first, fourth, ninth and so on—to ensure that selection is randomised.
In the beginning, we would sometimes fill 200 forms but only 150 people showed up.
While one person from the two-member team convinces the family member to sign the consent form, the other escorts them to the camp. We had to start doing this because in many cases, people would fill the forms but not show up at the camp. In the beginning, we would sometimes fill 200 forms but only 150 people showed up. They would say ‘our family isn’t allowing us to step out’; others would say ‘we have to go to the market now, we don’t have time’. So, it’s our responsibility to ensure that they reach the camp.
We can select only one person from each home for the survey and they have to be over 12 years old. For anyone between 12-18 years of age, we have to get the consent forms signed by their parents.
11.30 AM: I’m called by my volunteer to a home where the lady is refusing to sign the form. She tells us that she was quarantined earlier by the very same CHW who is at her doorstep now doing the survey. She says, “You will take our blood for testing and then quarantine us again. We don’t want that.” She isn’t the only one with this fear. The pandemic is at its peak, and the fear is palpable. In some cases, we aren’t even allowed to enter the locality because of similar apprehensions. I assure her that if she gets quarantined, she could inform me; that we were in it together. She agrees to sign the form, albeit reluctantly.
Her next door neighbour meanwhile wants to know why she’s not being called in for testing. We explain to her the ‘every-fourth house’ formula. She isn’t very happy with us either, since we’re leaving her out. “You come to us normally for teaching our kids or giving them vaccinating them; why aren’t you involving us now?”, she demands.
Either way, convincing people is our biggest challenge. In some cases where the corporator has goodwill, it’s easier because the people listen to them and we’re able to manage those communities.
12 PM: I get a phone call from yet another volunteer. One of his survey participants—a woman—has already donated a blood sample. But her husband and mother-in-law are furious with us and are demanding that we give back the sample.
1 PM: When people visit the camp, lab technicians from Thyrocare first verify the details of consent forms carried by the participants. The details are noted down—the participant name, age, travel history, and any interactions they might have had with people infected with COVID-19.
After logging in the data, the technicians draw 5 ml of blood from the participant. Each sample is then divided into two—one is taken to Kasturba Gandhi Hospital (KGH) in Mumbai and the other to Delhi.
One of the participants refuses to take the pen to sign. “It was used by the man in front of me, so it might be infected,” they say.
Since each camp has six technicians, most times participants don’t have to wait for too long, especially as they don’t all come at one time anyway. One of the participants refuses to take the pen to sign. “It was used by the man in front of me, so it might be infected,” they say. I sanitise it and give it back. Another man points out to me that the technician at one end of the camp hasn’t sanitised his gloves between patients. People are aware of the necessary precautions they need to take but our team still checks for masks and sanitisers.
2 PM: The team from KGH arrives. They come twice a day, once at 2 PM and then again at around 6 PM. The samples and forms are handed over; the hospital team counts both and verifies the tally.
6 PM: The KGH sample collection team arrives once more, to collect the rest of the day’s samples. As a field manager I have to be there till they leave. I wait till they are done, help the Thyrocare team and the CHWs to pack up, and only then do I leave for home.
7 PM: I reach home and it’s time for the daily planning meeting with the researchers from Tata Institute of Fundamental Research (TIFR), team members from IDFC Foundation and A.T.E Chandra Foundation who managed all the back-end operations for the study. We provide them a review of the entire day’s work. This includes updating them about the identification log—where volunteers are asked to note down the number of doors that are locked, how many people agreed to the survey, how many disagreed and their reasons for it. Because of the lockdown, many people left for their villages, and close to 30-40 percent of homes are empty.
After this call, we speak to the MCGM MOH (Medical Health Officer) since the health posts come under their purview. We tell them about the communities we plan to go next and enquire about their staff availability. We then inform Thyrocare about the next day’s meeting points.
1 AM: The calls and meetings are finally done and I can finally go to bed. I only slept for 5-6 hours each night and my mind was consumed by the survey. Towards the end, my health deteriorated.
My family asked me whether the survey would stop if I didn’t go for a day. I told them that I had responsibilities as a field manager of coordinating with various stakeholders, deciding what would be done on a particular day, and planning for the next. I couldn’t let the others down.
As told to IDR.
—
Know more
- Read about the results of Mumbai’s first sero survey.
- Read more on how the Mumbai sero survey results compare with what we already know about COVID-19.
- Read about results from the second sero survey conducted by Indian Council of Medical Research (ICMR) and what it indicates.





